Home /
Telehealth Impact: Rapid Transition in Response to a Pandemic
It’s no surprise, the pandemic changed everything across the nation. Centerstone was no exception. What was previously considered the future of community behavioral health care instantly became the present: telehealth and virtual patient engagement went from being a growing innovation to a necessity, virtually overnight.
In March, when COVID-19 hit the US and talk of national shutdowns began, Centerstone immediately initiated a transition from mostly face-to-face, clinic-based services to a primarily remote workforce and telehealth service delivery system. By the end of March, clinicians across the Centerstone system were working from their homes, and any patient who could be safely and effectively reached and treated via telehealth was offered telehealth services.
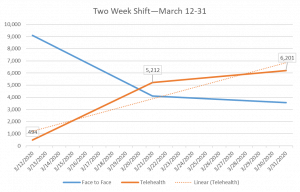
Between March 13 and March 31, Centerstone equipped over 3,000 staff to work remotely, held approximately 11,000 virtual meetings, implemented ‘virtual office hours’, and began refining related policies and procedures. The number of telehealth services provided increased from an average of 500 to 6200 daily. In April, Centerstone began seeking and securing federal funding to support COVID-related expenses, including telehealth transition work, and began examining options for an effective, long-term application and integration of telehealth services across its system. By June, with COVID-19 restrictions fluctuating across states, Centerstone was delivering 70% of services via telehealth.
To inform continued delivery and expansion of telehealth services, Centerstone’s Research Institute conducted a rapid evaluation of patient and clinician perspectives related to telehealth services and future preferences. Overall, we found that clients are extremely satisfied with how quickly they are able to schedule an appointment, prefer to receive services via telehealth in the future, and would recommend these services to family and friends. Clinicians report benefits such as decreased commute times, increased flexibility in scheduling, and improved access to hard-to-reach clients. They also reported patient barriers that impact care, including limited patient access to connectivity or technology, limited patient access to private space for sessions, and a low level of patient comfort using required technology. Using this and other information gathered by Centerstone and industry experts since March, Centerstone is continuing to refine its virtual service delivery approaches. The following outlines some examples of the improvements that have been made over the past several months.
Telehealth: 4 Clinical and Administrative Improvements Made in 2020
- Provider Training
- Telehealth Rooms Expansion
- Patient Engagement in Care
- Connect Telehealth Team
1. Provider Training
As the COVID-19 pandemic spiked in the mid and latter months of 2020, the demand on Centerstone’s existing telehealth technology platforms grew exponentially, as did the urgency to expand the number of providers skilled at delivering virtual care. More than two decades of related pilots and enhancement/expansion projects across the Centerstone system made it possible to rapidly ramp up these services, as well as the number of skilled providers. Doing so required a two-pronged training approach, with one focusing on the technology and the other focusing on effectively delivering evidence based care in a virtual environment.
During the early March emergency response activities, subject matter experts from Centerstone’s Research Institute, administrative leadership, and IT department developed and delivered trainings on how to effectively use the telehealth technologies that had been piloted within our system. These trainings were provided within the first few days of ‘work-from-home’ mandates and were accompanied by information to help patients secure internet access and devices (e.g., free or low-cost internet/Wifi, location of open hot-spots, device offers, etc.). Research Institute leadership and subject-matter experts also provided staff with scheduled and on-demand consultation, as well as resources such as user guides, FAQs and training videos containing strategies for delivering best practice/high quality care via telephone and televideo platforms. Some of the training modules developed and delivered in response to the immediate demand are listed to the right.
2. Telehealth Rooms Expansion
Prior to the pandemic, Centerstone piloted and was strategically expanding telehealth rooms in local clinics. This model dedicates private rooms within clinics where patients can access specialty care delivered by remote providers. The rooms are equipped with telehealth technology and furnishings that support effective care delivery. Initially, this model was integrated to ensure that patients could access needed specialty care, particularly increasing demand for limited psychiatric services.
The pandemic created a broader need for patients to have access to all levels of care with as little personal contact as possible. In response to the pandemic, Centerstone initiated a rapid scaling of the telehealth room model across the system and now has 54 fully equipped telehealth rooms with modern, approachable technology (e.g., mounted TV’s, cameras, audio, etc.) and 64 private rooms that use mobile carts or iPads within clinics. Expansion of this model has helped to address some of the barriers to care that patients and clinicians have encountered related to virtual services, including patients having issues with access to private space in homes for virtual sessions, as well as patients having limited access to required technology and/or internet connectivity. The rooms are managed by onsite staff and are equipped with personal protective gear aligning with CDC recommendations to maintain safety for staff and patients.
Clinical Education Training Developed and Delivered in Response to the Pandemic March 13 –April 13, 2020
- Conducting Telehealth with Older Adults
- Telehealth Transition: Evidence-Based Strategies for Engaging Young Children
- Telehealth Transition: Evidence-Based Strategies for Engaging Older Children and Youth
- Crisis Intervention and Response via Telehealth
- Incorporating Worksheets and Treatment Aids into Telehealth
- Group Therapy via Telehealth
- Navigating Licensure during the Transition to Telehealth
- Translating CBT to Telehealth
- Overcoming technology access and barriers
- Navigating Confidentiality and Privacy
- Structuring Telehealth Sessions with Children, Youth, and Families
- Balancing Family while Working from Home
- Life Skills Teaching via Telehealth 1
- Life Skills Teaching via Telehealth 2
- Life Skills Teaching via Telehealth 3
- Conducting Marriage and Family Therapy via Telehealth 1
- Conducting Marriage and Family Therapy via Telehealth 2
- Conducting Marriage and Family Therapy via Telehealth 3
- Ask the Experts – Conducting Marriage and Family Therapy via Telehealth
- Virtual Office Hours
3. Patient Engagement in Care
Prior to the pandemic, Centerstone was piloting a virtual patient engagement model within one of its call centers. At the onset of the pandemic, key elements of that model were rapidly scaled to support and accommodate the substantial increase in requests for scheduled appointments. Inquiry call volume increased by 44% between May and October, with more and more callers expressing an urgent need.
In response to the growing need, Centerstone launched a single, national phone number, 877-HOPE123 and strategically integrated patient engagement model strategies within the system. These measures provide potential patients, their loved ones, and referral sources efficient access to services and related information.
The patient engagement model includes:
- Qualified, skilled agents managing phone lines and written inquiries made using the centerstone.org website
- Telephone engagement, information sharing, and triaging to programs and services
- Appointment scheduling
- Consistent follow-up contact with patients until appointment
- Metric reporting for call center measures that are available in real-time using a dashboard created by Centerstone Analytics and essential to managing this important support service
This model maintains a strong focus on helping the people access the individual level of care needed as quickly as possible. The pandemic created clinical and community conditions that necessitated rapid refinement and expanded implementation of this model, including deployment of equipment and technologies to create seamless connectivity for the agents, as well as back-up/fail-safe technologies. Additionally, the expansion necessitated rapid recruitment, onboarding, and training of call center agents to meet virtual care needs across the Centerstone system. Daily Flash Reports were also developed to provide analytics to inform system management, including call volume, speed to answer, abandonment rate, and intake appointment rates.
4. Centerstone Connect Telehealth Team
A key element of patients successfully accessing and benefiting from telehealth services is the clinician’s and the patient’s ability to use the required technology. As such, Centerstone has established a dedicated team to complement the Call Center patient engagement model and overall virtual service delivery. The Connect Telehealth Team supports staff and patient use of telehealth technology platforms and software. It serves as the “Tech Desk” for all staff and patients to ensure that they are able to deliver and receive care as seamlessly as possible. The team is readily available to assist with multiple areas, including to:
- Troubleshoot issues related to Intake and appointment scheduling within telehealth platforms
- Optimize software platforms to help increase functionality
- Directly assist patients (new or active) with connecting to telehealth appointments (e.g., software downloads, training on software use)
- Provide an introductory “Tech Session” for new patients (a test run prior to the actual clinical session)
For more information about the Centerstone Connect Telehealth Team or Centerstone’s evidence-based clinical trainings, please contact CenterstoneDigest@Centerstone.org.
Moving Forward
As the potential for an end to the pandemic increases, Centerstone continues to make patient and staff health and safety the highest priority. Moving forward, Centerstone is continuing to research and integrate new innovative and effective ways to deliver care that changes people’s lives, particularly in the face of any obstacles that may arise.
